Recovery from Traumatic Brain Injury Requires a Coordinated Effort
Team Approach
By Mark Morris

In the U.S., 2.5 million adults and children sustain a traumatic brain injury (TBI) every year.
The Brain Injury Assoc. of America (BIAA) reports that more than 2 million of those injuries are treated in emergency departments, while approximately 50,000 result in death. Nearly 280,000 are admitted to hospitals, after which patients transition to inpatient rehabilitation, where the goal is to get back to their maximum level of function and independence.
But what’s involved in that rehabilitation process for brain injuries? It depends on the patient.
“Many people associate traumatic brain injuries with a younger population because they tend to engage in riskier behaviors. Older people who hit their heads from slips, trips, and falls are also susceptible to TBIs,” said Jennifer Blake, an occupational therapist with the inpatient program at Weldon Rehabilitation Hospital, adding, however, that anyone at any age can sustain a brain injury.
The Centers for Disease Control and Prevention (CDC) defines TBI as a “disruption in the normal function of the brain that can be caused by a bump, blow, or jolt to the head, or penetrating head injury.“
Traumatic brain injuries are evaluated on a spectrum, said Blake, noting that someone who experiences a concussion, also known as ‘mild traumatic brain injury,’ can usually return to normal with just limited therapy. On the other hand, people with moderate to severe brain injuries require medical care and more comprehensive inpatient rehabilitation. Often these patients need some level of supervision after discharge.
On occasion, someone may have a head injury and not immediately recognize it. For example, if a person is in a car accident and has a broken leg, that might get the primary treatment focus, Blake explained. Even after a CT scan, the brain injury may not initially show up. “It’s only after further investigation, when the person is having trouble concentrating or paying attention, that they discover the brain injury.”
Because our brains are essential to all our physical and mental functions, therapists have found that taking a multi-disciplinary approach yields the best results in helping people recover from a brain injury. A team of physical therapists, occupational therapists, and speech pathologists, supported by 24/7 care by medical staff such as nurses, doctors, and pharmacists, make sure all the patient’s needs are addressed.
Because our brains are essential to all our physical and mental functions, therapists have found that taking a multi-disciplinary approach yields the best results in helping people recover from a brain injury.
“We meet once a week to make sure we are all on the same page,” said Julie Bugeau, an occupational therapist for Encompass Health Rehabilitation Hospital of Western Massachusetts. “We have an open discussion to determine where the patient is in terms of therapy and function. We also ask questions outside of the therapy, such as, ‘how are they medically?’ ‘Are they eating well?’ We try to look at all the factors that can affect their rehab.”
What’s the Plan?
Blake said most admissions in the inpatient setting last only two weeks, so working as a team helps them determine the patient’s eventual discharge plan.
“By working together in an interdisciplinary team, we can figure out what’s working, what’s not, and make changes along the way.”
Blake said an individualized plan for rehabilitation is developed by therapists who work with patients in three key areas:
• The physical therapist studies a patient’s mobility: for example, how well they can get from one place to another, their balance, and how well their motor skills can function;
• The occupational therapist helps patients with self-care skills, such as eating, getting dressed, bathing, as well as tasks like cooking, cleaning, and managing medications; and
• The speech and language pathologist addresses higher levels of cognition, such as memory, attention, concentration, problem solving, and decision making. Sometimes the pathologist works with patients whose brain injury causes dysfunction in producing or understanding language.
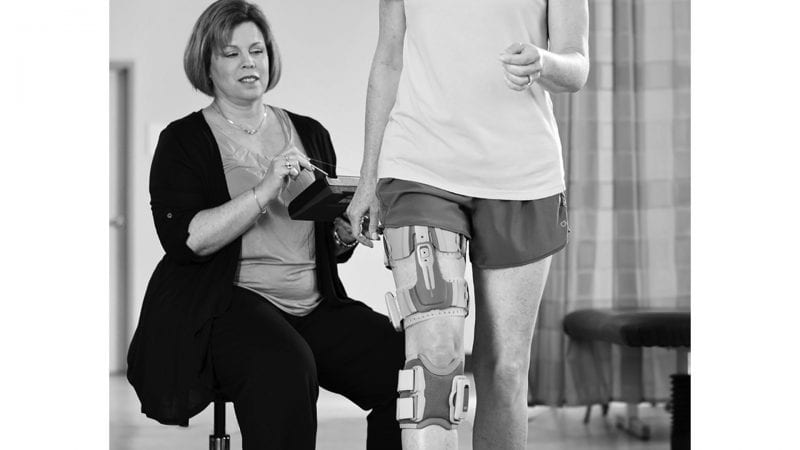
Advancing technology offers therapists tools to aid in rehabilitation that were not available years ago. Bugeau discussed how devices such as the Bioness L300 and H200 help brain-injury patients regain the use of their legs and arms. The L300 attaches to the leg and, through electrical stimulation, can aid a person’s ability to walk.
“The idea is that, with repetition, those leg muscles will be able to move properly without the external stimulus,” she explained.
Meanwhile, the H200 helps re-establish the movement of arms and the grasping action of hands. Bugeau said using these devices results in positive responses from her patients.
“We’ll have patients who say, ‘my arm doesn’t work — I have a dead arm,’” she noted. “Then, when they see their arm move and their hand open and close, it boosts their confidence and makes them feel more hopeful; you can see it in their faces.”
By employing the different therapies, Bugeau went on, the hope is to maximize the patient’s abilities. But, she added, “while the therapy is important, rest is also an important part of the recovery.”
While many patients transition directly from inpatient to outpatient care, Bugeau said Encompass also offers a home-care component for those who are not yet ready to make the move.
“We’ll have patients who say, ‘my arm doesn’t work — I have a dead arm.’ Then, when they see their arm move and their hand open and close, it boosts their confidence and makes them feel more hopeful; you can see it in their faces.”
“We will help patients settle into their home and continue training with them and their families to make sure they are safe and getting stronger,” she said. “It’s an option we recommend until the patient is ready to move into outpatient treatment.”
Blake added that the outpatient phase of care at Weldon involves working closely with families during outpatient therapy to help them manage that part of the process.
“Let’s say a patient is receiving all three therapies in an outpatient setting,” she explained. “We will try to schedule all of them on the same day to make it a little less overwhelming for the caretaker.”
Blake said it’s important for the injured person and their support group to understand that, when a person suffers a brain injury, it can be a difficult adjustment for everyone involved.
“You can’t see the residual impairments from a brain injury,” she said. “The person might experience a personality change, or a once-independent person may now need lots of assistance with daily life.”
That’s why Bugeau’s staff involves the patient’s family in training and education early in the process. She said the classes help the family understand how their loved one’s brain injury is progressing and how to properly handle behaviors that are out of the norm.
“We make sure to screen every patient with a brain injury for depression because it is a such a common symptom associated with brain injuries.”
Steady Improvement
While plenty of information and support are available for families, Bugeau said the trick is not to overdo it.
“We create a folder with specific, individualized information that is appropriate to the patient’s injury. We don’t want to overwhelm the family, but we want to make sure they have the information they need.”
Blake and Bugeau encourage families dealing with a brain-injured loved one to take advantage of the support groups available at their respective organizations. Weldon offers a faith-based group as well. Both therapists also cited the Brain Injury Assoc. of Massachusetts as a solid resource for families.
In all cases, the goal is helping patients with a brain injury get back to a maximum level of function and independence.
“It’s hard to say how much time each person needs,” Blake said. “And while things can change quickly or gradually, people do improve and get better.”